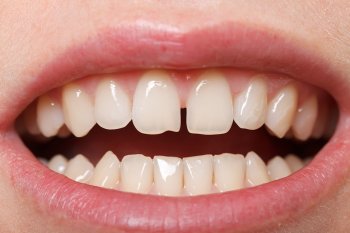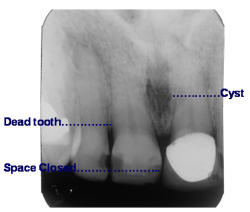
While dentists look at the x-rays of the diastema space, they do not notice the necrotic central incisor and the midline cyst in the nasopalatine bone. It was interesting to notice that dentists did not notice this pathology, and then, exciting to develop a nonsurgical treatment that resolves both the incisor and cyst. (Figure 1)
The classic induction theory analyzes experimental findings and designs theories to explain empirical patterns. The d eduction theory begins with accepted principles or postulates and deduces them to consequences. Clinical dental practices blend both approaches. Dentists with decades of experience tend to employ their experimental findings on patients and find fixed indicators upon which to construct modalities of daily practice, while others depend more on deductive postulates in order to construct theories. Some dentists may become convinced of an apparent valid postulation before consideration of extensive experiments and consistent results.
To a large degree significant advances in understanding dental science have been formed out one’s intuitive grasp of specific indicators of infection within the large complex of facts which reveal a basic hypothetical law, and from this, determine conclusions. Indicators of infectious tissues are many and can be confused. For a “scientific realist” such as a dentist, an underlying hidden reality may exist within the principle concept or theory, and yet, at the time that reality may be beyond the dentist’s ability to observe it or measure it. Consequently, during the development of a complex theory or practical dental method, a practitioner may be momentarily stumped by the diastema and the complete solution may come much later. In the case of Osteo-Endo-Cystic Therapy, (OECT) this is what happened in the 1970s. Indicators began to emerge.
Indications of the Diastema Dilemma
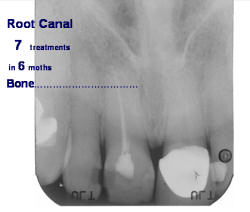
Midline spacing, dentition deviations, decrease in vitality of maxillary centrals, root divergence (#8-9 PA x-ray), gingival cleft, discoloration of one central, constant calculus on mandibular anteriors, enlarged “fat pad” lingual to #8-9, sensitive apical palpation or percussion to maxillary centrals, enlarged “incisive canal,” unusual sensations in that area, history of thumb sucking, smoking, periodontal problems and extensive dental restorations.
In the decades of the 1970s and 1980, the use of calcium materials were being significantly validated by nonsurgical endodontic therapies [1] while the Calcium Therapy Institute moved into calcium methods of nonsurgical periodontal therapy. [2] Both the periodontal and the root canal therapies were fused into the method of cystic therapy as reported in the 2009 ConsEuro Journal of Clinical Oral Investigation, an abstract of this paper which offers an original framework for understanding periodontal disease and other oral conditions or deviations. (Figure 2)
METHODS and MATERIALS
It is not necessary to scrap the assertions, theories, or body of findings on cystic formations in the nasopalatine tissues. In fact, when one ponders the historic studies of Dr. Roberto Holland et al of Brazil and others, as well as the abundant experiences compiled from clinical applications of timed-release calcium compounds, it becomes prudent to be in useful agreement with them and be aware of the significant properties of calcium by considering these findings more broadly. Then, the diastema deviations can no longer ascribed as innocent and relegated to cosmetics, only to be ignored.
Our traditional dental conventions ascribe no common cystic formation in the anterior nasopalatine bone of the maxilla, and yet Calcium Therapy Institute dentists find diastema spacing, maxillary central deviations, and the nasopalatine cyst are common and far from innocent. The components are complex, long-term infectious conditions for the entire oral cavity. Furthermore, it becomes obvious that the cyst and a central incisor are directly related. There is an immediate and substantial relation between the two, resulting in one of the major causes of periodontal disease, rampant decay, calculus formation, and assorted dental breakdowns. The diastema in the maxillary arch is noticeably unilateral to the midline and rather subtle in appearance. On the other hand, spacing may occur in the mandibular arch but is most often bilateral and without particular damage to a single incisor. The history of therapy for the maxillary anterior condition is hardly acceptable. Rarely does anyone believe the cystic formation exists there. Dentists have been taught that it does not, so by the time therapy is recommended, the pathology has become so blatantly apparent and long-standing that it cannot be ignored. The diastema space widens, the anterior teeth deviate from the midline, destruction has spread to the entire anterior segment of the maxilla and its dentition. The prolonged full-mouth breakdown by then is intolerable. Meanwhile, the cyst persists and gradually kills at least one of the incisors.
Long ago researchers found that a nasopalatine cyst is caused by epithelial formation in utero that forms from remnants of the maxillary bone tissues at the midline fusion point. These cells proliferate to form a duct lined with epithelium and eventually migrate inferiorly between the centrals. In youth these cells give off toxins which are excreted into the mouth through the “incisive canal.” It is not clear what factors initiate this flow pattern. The cystic formation is soon invaded by oral bacteria and their toxins also exit to the mouth. [4] [5] [6]. This situation sets up ideal conditions for long-term dental infections in youth and throughout adulthood, esp. upon the necrosis of one of the centrals.
Another Calcium Therapy Institute finding is the odontogenic connection. Nasopalatine duct develops, becomes infected, drains and expands within the maxilla as a cyst densely encapsulated, moving bone and teeth alike, hence the diastema. Soon, an incisor is victim to the toxic concentrate. Although there is general acceptance to the contrary, there seems to be no direct genetic predisposition for the spacing, the cyst, nor the necrotic tooth. But the common rate of occurrence, the locale and the lack of pain experienced by the patient would seem to belie the presence of dental concern other than cosmetics. There is no pain, just teeth out of place. So let’s move them back or close the space. The full consequences of this become quite apparent in later life. The so-called diastema phenomenon has been around so long, is so prevalent and described in literature for ages as innocuous that it is generally belied and endured as a distinguishing genetic characteristic. So what’s the problem?
The size, locale and occurrence of these conditions seem incidental until it is quite late in its progression and clear we are dealing with a large, non-vital maxillary central incisor and a cyst the size of a small almond which has developed in the maxilla for 20 years or more. Were this sort of infection located on radius of the forearm, slowly enlarging, draining out of the arm and painless for 10 weeks, someone people would be rather upset about it. Few would tolerate it. And yet, the diastema dilemma is routinely, inadvertently hidden upon orthodontic closure of the space, upon placement of crowns or proximal restorations. These only conceal the problem and do nothing to resolve the issue. Consequently, the pathological discharge and its dilatory affects are right in front of us. We have taught ourselves to not see it. Unfortunately, over years of clinical experience it became evident that root canal therapy of the necrotic central, removal of it, surgical intervention on the cystic area, or all of these together would not prevent the cystic regeneration.
However out of these trials and results the Calcium Therapy Institute designed a non-surgical calcium therapy for both the tooth involved and the accompanying nasopalatine cyst. The condition of diastema spacing or deviation is solved with nonsurgical Calcium Method of Osteo-Endo-Cystic Therapy. Upon utilizing varied formulae of weekly or monthly applications of timed-release calcium/zinc/ester compounds directly to the infected tissues, without local anesthesia, rapid healing is stimulated. The most critical and unique aspect of the Osteo-Endo-Cystic Therapy is consistent on-site monthly treatments over eight to twelve months or the lesion will not adequately heal. This may seem contrary to the three-month recovery period for the bone. Nonetheless, it is invariable the in this system more recovery time is a dominate consideration. And yet, it would be normal when account is taken of the common clinical finding that after obturation it takes nearly a year for a root canal apex to fully accomplish closure.
Over four decades standard methods were developed, measured and analyzed in to a system based on statistical research from around the world. Soon a practical modality was employed and continually re-evaluated. The healing response is rapid and otherwise uneventlful, therefore the cycle of repetition quickly verified the statistically significance of each method. Since the outset the patient acceptance has been extraordinarily high after commonsense information on the protocol is explained and understood.
RESULTS
A major result of adopting as well as constantly re-evaluating traditional and current thinking about the diastema situation has forced the design of new theories and methods that resolve this complex condition in a commonsense manner. A rather routine example of the protocol is:
- Diagnosis from specific indicators (a diastmea, tooth discoloration, lingual “fat pad” etc)
- Verification ( cold test of centrals, palpation of labial fold, periapical x-ray, root deviation, etc)
- Anesthetic, nonsurgical endodontia on involved central, and initial calcium application
- Monthly subgingival calcium treatments of maxillary anterior quadrant
- Continued calcium treatments for 8 to 10 months, follow indicators, 6-month post-op x-ray
All of the above may vary with each case depending on the patient’s capacity to respond and the ability to listen to them. Here is a perfect example:
A very healthy 21-year-old female presents with no problems whatsoever. At the end of her every- 4-month cleaning and exam, she casually comments that she is still wearing her orthodontic retainer, after eight years. Why? Without it her upper central moves within a week. As a child she had a space there and is rather unhappy with her orthodontists about her years of two sessions of braces. He is also concerned that the retainer is not worn enough. The inflammation of tissue lingual to the upper centrals is periodic and just normal.
A quick cold test of the central reveals one is non-responsive and the other only slight so. The periapical x-ray shows a large dark area between the centrals with one of the roots diverged. She could see both immediately. Even at her age the constant drainage and dental breakdown is fully established. However there was no reason for the riff between the patient and the orthodontist because the entire condition can be resolved with a little anesthesia, a non-surgical root canal and a series of direct two-minute calcium treatments. This may take monthly treatments over a year, but it will preserve all the beautiful and conscientious dental care.
The most common visible indicator is the diastema space. A conservative Calcium Therapy Institute estimate of this occurrence in a general dentist’s patients is 50%, and in an orthodontist’s and a periodontist’s patients must be 60% and 70 percent. In other words, the diastema problem may amount to the most common cause of complete dental breakdown. Beyond that, the Calcium Therapy Institute has found that aspects of the clinical uses of calcium materials touches every field of dentistry from Operative, Endodontia, Periodontics, Occlusion, Orthodontics, Implantology, and presently Osteo-Endo-Cystic Therapies. Over the last 45 years large resources of cases have been accumulated which were initially diagnosed by competent dentists as “hopeless” with periodontal disease far beyond their ability to preserve the remaining teeth. Each case was individual and had a specific protocol for success in saving almost every tooth, and most involved the diastema dilemma.
Every few years a new door was opened with an answer, only to find more doors with questions, but never so profound as a solution to the diastema. Today these calcium materials can be utilized on every patient in the general dentist’s practice.
In the 1960s the Calcium Therapy Institute began to conduct clinical trials, laboratory studies and seminars employing several of the calcium compounds. Since the mid-1970s specific details of calcium applications in dentistry have been presented personally in clinical settings and at dental or educational gatherings around the world. By 1995 the information has been available on line and a 60-page, seven-session manual was compiled for teaching online or in person. Accordingly, patients make themselves available for the calcium therapies around the world and over the Internet, and in one general practitioner’s office over 60 cases are seen a month. Calcium materials are also provided for homecare maintenance.
The most gratifying result of Osteo-Endo-Cystic Therapy is the remarkable improvement of the oral cavity and how that affects the physiology of the entire body. Patients who have experienced the recovery of a tragic dental situation are far more interested in continuing their dental care and see the value of putting their dental structures in better order. Two of the striking results are the lack of constant calculus buildup on the lingual of the lower incisors, and healing of the gingival “fat” pad lingual to the upper centrals. This fat pad becomes a “flat” pad of tough, fibrous light pink coloration like the rest of the palatal tissue. The long-held notion of a “fat” pad is a misnomer and a sign of infection. Thus, the dramatic reduction of the calculus and a flat pad are indications of successful healing of the cyst in the nasopalatine area. This merely confirms that such areas of the oral cavity should be the most resistant to infection due the copius salia flow and tongue function there. It is like releasing two of the most powerful preventive elements of a healthy oral condition. Without either it would be difficult to adequately restrain any form of bacterial invasion to the body’s digestive system.
DISCUSSION
There are at least two common assumptions here. The diastema deviation condition is not pathological with no concern for therapy. There is no cyst. Second, there is no odontogentic relationship between the maxillary bone and vitality of the upper centrals. Dental literature is replete with comprehensive surgical procedures to resolve either the endodontic destruction or the osteous collapse of the nasopalatine area. In many cases the surgical intervention needs to be repeated and there is loss of one or several incisors. On the other hand, there is abundant information from hundreds of cases by dentists that both are mere assumptions. Upon showing diagnostic periapical x-rays to hundreds of dentists, virtually all see nothing. All agree nothing is wrong, no pathology of the osteous tissue between the centrals, no cyst, and no therapy needed. Inadvertently, dentists think and read x-rays with an “odontogenic eye,” i.e. of and by the tooth. Even radiologists have been taught by dentists to “see” the same thing, nothing. They respond that such dark areas appear on MRIs all over the skull. And they do. On the contrary and almost invariably, patients see exactly what is in the x-ray, a dark area of infection that is pushing the teeth around. They also see a distinct incisive duct, not a canal, between the centrals draining into the anterior palate. This may house the nerve and vessels for the palate, but it is also a perfect vehicle for constant drainage of toxins and the reason for easy invasion by bacteria. So, the patient wants to know why their perfectly healthy upper central has no vitality, no pain, no reason for concern, but it needs a root canal, when there seems to be no infection anywhere, just calculus all the time on the lower incisors.
If so, why is it that when treated with a little calcium, the entire area feels better in a few moments? And with complete root canal obturation and calcium treatments the symptoms that they didn’t even know they were tolerating are gone, the fat pad is now flat, and the dark area is filled in with a latticework of bone. What is that black area between the teeth? Is this a sinus? A sinus at that area of the midline has been reported so rarely the question is moot. And what happened to the calculus deposition on the lower incisors, where most saliva flows in abundance? At first the calculus becomes less dense and whiter, and then no longer deposits on the teeth. Even the gingival cleft around the central at the drainage point heals. Maybe it’s due to better oral hygiene. Possibly, but experience has shown that calcium treatments of the maxillary diastema alone quickly result in a reduction of calculus, esp. on the mandibular incisors.
Upon consideration of both evidence-based and outcome-based clinical research over 30 years of the specific diagnosis and treatment in the clinical setting, there appear pre-eminent markers that apply to almost every case. The most interesting aspect is that there are two distinct conditions that must be dealt with and it remains speculation as to which is the instigating culprit, “the chicken or the egg.” In this instance, is the cyst formation the cause of the non-vital tooth, or is the necrotic tooth the cause of the cyst? At this juncture the culprit appears to be the cyst. Regardless of the answer one thing is clear.There are two components to these diastema deviations and infections. They both need attention for complete healing and recovery. Neither is innocent and they are ignored at the peril of complete dental devastation.
Having been steeped in this arena prior to the 1980s with the only choice of treatment being surgery, it was common to refer patients with severe diastema problems to the oral surgeon. After nearly 12 years of this approach, to his distinguished credit, our favorite surgical specialist informed us that he could no longer perform the extensive nasopalatine surgeries we requested. They were not working. If a single cell of the cyst were to survive the surgery, in a relative short time the cystic cells replicated, re-establish themselves, and infection ensued. As this situation sunk in, the questions remained. How do we resolve this complexity? Which is the actual cause? Which the victim? Which do we start with? And especially, what do we treat with? The endodontic half of the situation was and remains the rather simple, straightforward part. Perform a root canal on the necrotic tooth, usually the simplest in the mouth.
Based on clinical experience with unique timed-release calcium materials with the capacity to provoke gingival and perioapical recovery, their applications were found to have significant rapid tissue healing and high coefficients of safely. The decades since have contributed immensely to the knowledge of the benefits calcium provides to control bacteria of the mouth and stimulate oral tissues for long periods at a time. This evidence and assertions led to constructive conclusions yet to be fully understood.
CONCLUSIONS
The essence of this paper is simple and based on simple facts. Calcium is the most common mineral in the body, essential in cell and organ regulation of virtually every biological process. It is a powerful tool in soft tissue regeneration. Merely one percent of the calcium needed by the body comes from foods. The other 99% must come from the bones. Free calcium has not only a huge inherent impact on dental and facial bone, but also on reducing the affects of biophosphonates used in attempts to prevent osteoporosis. Routine applications of timed –release calcium materials most likely would contribute considerably to calcium levels of the bones, esp. the alveolar and basic bones of the jaws and face, where by the way, the body tends to go first and foremost when in need of calcium.
The most recent insights by the Calcium Therapy Institute look toward the concerns of calcium deficiencies with our view through the “periodontal window.” The oral cavity is not only the front door of the digestive system, but the open “window” to the body’s system by direct route of the periodontium. Serum calcium studies have shown clear evidence that free, timed-release calcium is rapidly and safely absorbed by the periodontium in high concentrations over long periods of time as employed in these non-surgical periodontal and cystic therapies. The same is known of the dense enamel and other dentition. Calcium penetrates these structures freely and efficiently, just as nitroglycerine tables are employed under the tongue, rather than swallowed, to reach the heart in seconds, through the periodontal window, to reduce angina pain.
Furthermore, lactose intolerance conditions are readily viewed as calcium deficiency problems. Its negative effects on the oral cavity are horrendous. The digestive system loses its ability to breakdown lactase into glucose and galactose due to the lack of lactase enzyme in the small intestine. This intolerance has as much to do with calcium as anything. Bacteria can break down the lactase enzyme which reduces the enzyme’s essential need to stimulate the lactose breakdown for proper digestion. This leaves excess lactose in the stomach and intestines which increases the migration of lactose into the large intestine and excessive overgrowth of bacteria throughout the entire system, the colon, the lungs and regurgitation back into the mouth resulting in bad breath and intolerable levels of bacteria for the periodontium to deal with.
The introduction of safe, efficient timed-release calcium materials to this dynamic process would result in better digestion. Second, it would be beneficial in reducing bacterial replication and allow the healthy tissues to regenerate with a most essential mineral, calcium. This is taken from another Calcium Therapy Institute study that showed that calcium materials do not “kill kill, kill” so much as inhibit the replication of bacteria over long periods. It was years into use of these calcium compounds that this singular finding securely established their efficacy as non-invasive materials for human application.
Therefore, the clinical uses of calcium materials would seem to be a high priority for such otherwise invasive periodontal therapies, surgical or non-surgical. The calcium Method of Osteo-Endo-Cystic Therapy poses an entirely advanced level of periodontal therapy as well as an excellent source of calcium. On a practical, clinical level, dentists would best be attentive to research of any kind this arena, esp. regarding the periodontal window. Hygienists would quickly be attracted to calcium use in their profession. Every dental hygienist would be an immediate benefactor of calcium materials. Their need for anesthesia would virtually disappear. Also, orthodontists would soon eliminate the term “ortho relapse” of cases. One of the exquisite sidelines to the extended calcium applications is that it literally stops the movement of a tooth under the influence of infection. Then, as the endodontic infection heals, the teeth can be moved with orthodontic appliances to where they belong, under the “protection” of calcium treatments.
The continued grasp of dental research in the calcium therapy of the diastema dilemma would be a lapniappe, a pure gift of leverage toward clinical success. Certainties, validity and determinism are not mutually incompatible, so we can safely promulgate the protection of the older orders of dental science. No solid dogma is based on authority alone. No dental principle is fairly based merely on rank in the science. No biological methodology or dental theory need be based on who discovered or developed it. Only more conscientious research and clinical success will suffice. Osteo-Endo-Cystic Therapy poses a quantum leap forward in finding the significance of what dentistry has discovered about calcium.
ACKNOWLEDGEMENTS
Holland R. DDS MS et al, Brazil: Steg T.B. DDS, Higgins L.T. DDS MS & Lynch B. DDS MS, Nebraska: de Graw W. PhD & Sullivan D. PhD, Nebraska University: Chunawalla Y. DDS MS, India: Kominski A. DDS, Poland: Truka K. DDS, Iowa: Winick R. & Golden L. New York: Munro-Hall G.& L. England: Eakins G. MD & Dehning M. MD, Nebraska: Manassero A. PhD & Murillo E. France: Evans S. DDS, Missouri: The author has designed, produced and taught non-surgical calcium methods and materials in dentistry over 48 years around the world without formal financial support or conflict of interests.
REFERENCES Available upon request.
Author
Mark J. Manhart DDS Private practitioner since 1962, Director of the Calcium Therapy Institute, Former Associate Professor of Endodontia Creighton University School of Dentistry
Examples of Diastema Space
There are so many people, and I mean very famous people, who have the spacing in the front teeth that is really infectious and causing complete dental breakdown. They wonder why they need so much dental work, so much orthodontic braces, so many implants….. none of which solve the cyst and dead tooth problem of the “diastema” right under their nose between the front teeth.
Here are only a few:
- King Harald V of Norway
- Sir Elton John
- Gen. Colin Poewll
- King Juan Carlos of Spain
- The Prime Minister of England
- President of France
- George Bush
- many Hollywood stars
- and watch TV – you will see them all over the world.